- Updated on September 13, 2020
![]() By Dr. Artour Rakhimov, Alternative Health Educator and Author
By Dr. Artour Rakhimov, Alternative Health Educator and Author
- Medically Reviewed by Naziliya Rakhimova, MD
Here is the YouTube video “Heavy breathing at sleep“. This video clip has information and quotes from medical studies, which are described above.
 The effect of heavy breathing during sleep explains decades of medical research and clinical observations that sleep and especially early morning hours (4-7 am) are the times of highest mortality rates for patients with asthma, angina pectoris, stroke, seizures, and many other health conditions.
The effect of heavy breathing during sleep explains decades of medical research and clinical observations that sleep and especially early morning hours (4-7 am) are the times of highest mortality rates for patients with asthma, angina pectoris, stroke, seizures, and many other health conditions.
Asthma
American pediatricians from the Washington University School of Medicine in St. Louis in their publication noted symptoms related to bronchial asthma are often more prominent during sleep. These scientists found reduced lung function results (PEF and VEF) in the early morning hours (Porter et al, 1999).
 A group of Brazilian medical scientists investigated, according to their title Morning-to-evening variation in exercise-induced bronchospasm (Vianna et al, 2002). Their objective was to test morning vs. evening exercise-induced bronchoconstriction, as well as MV (minute ventilation) during physical exercise. The results confirmed that morning parameters were worse: FEV1 was significantly lower during early morning hours, while minute ventilation was higher meaning heavier breathing through narrower airways.
A group of Brazilian medical scientists investigated, according to their title Morning-to-evening variation in exercise-induced bronchospasm (Vianna et al, 2002). Their objective was to test morning vs. evening exercise-induced bronchoconstriction, as well as MV (minute ventilation) during physical exercise. The results confirmed that morning parameters were worse: FEV1 was significantly lower during early morning hours, while minute ventilation was higher meaning heavier breathing through narrower airways.
Over 30 years ago the Thorax published a study: Physiological patterns in early morning asthma (Hetzel, et al, 1977). The goal of the study was also to explain the sudden nature of some asthma deaths since, as these researchers discovered, these mortality cases often occur during early morning hours.
COPD
Several other publications were devoted to the effects of sleep on patients with COPD (chronic obstructive pulmonary disease). American scientists from the Yale Center for Sleep Medicine (Yale University School of Medicine, New Haven) wrote that COPD symptoms during sleep are common in patients with moderate and severe COPD, especially in the elderly. They experience stronger hypoxemia (reduced oxygenation of the arterial blood). In conclusion, it was stated that sleep has “profound adverse effects” on respiratory parameters and the exchange of gases (oxygen and CO2 in alveoli) in patients with COPD (Urbano & Mohsenin, 2006).
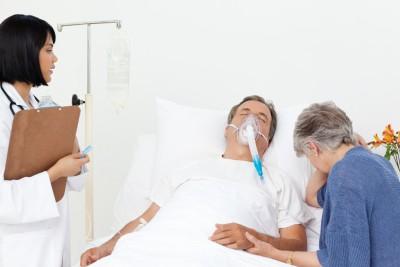 Moreover, Sheppard and colleagues in the publication from the Chest magazine noted that epidemiologic research has revealed that patients with COPD have higher mortality rates during the early morning hours (Sheppard et al, 1984). The load on the heart muscle during episodes of nocturnal hypoxemia, according to their conclusion, can be “as great as during maximal exercise”.
Moreover, Sheppard and colleagues in the publication from the Chest magazine noted that epidemiologic research has revealed that patients with COPD have higher mortality rates during the early morning hours (Sheppard et al, 1984). The load on the heart muscle during episodes of nocturnal hypoxemia, according to their conclusion, can be “as great as during maximal exercise”.
Coronary spasms and cardiac arrest
If patients with pulmonary conditions can die due to heart problems at night, what about heart patients themselves? This team of scientists found that coronary artery spasm is most likely to occur “from midnight to early morning” when the person is at the state of rest (Yasue & Kugiyama, 1997). This Japanese study was published in the Journal of Internal Medicine. The main and the only sleep-related variable and cause of these spasms is heavy breathing.
Intensive care professionals from the Department of Anaesthesia and Intensive Care Medicine of the Hadassah Medical Centre in Jerusalem, Israel also decided to investigate, according to their title, In-hospital cardiac arrest: is outcome related to the time of the arrest?
 These health professionals tried to find out if outcomes from in-hospital (CPR) cardiopulmonary resuscitation is different when it takes place at night. It was concluded that resuscitation during night shifts has poorer outcomes (Matot et al, 2006).
These health professionals tried to find out if outcomes from in-hospital (CPR) cardiopulmonary resuscitation is different when it takes place at night. It was concluded that resuscitation during night shifts has poorer outcomes (Matot et al, 2006).
Turkish cardiologists from Ankara published a study with the goal to explain the morning increase of sudden cardiac death. Their hypothesis was based on the role played by the sympathetic nervous system (Batur et al, 1999). It is known that the sympathetic nervous system drives respiration or minute ventilation up, thus, causing tissue hypoxia induced by hyperventilation.
A group of American cardiologists from the Georgetown University Medical Center in Washington, D.C. was also interested in the most likely time of death in 96 of the 139 patients who died suddenly. They found a distinct peak in death rates during morning hours (with high significance p = 0.04) (Behrens et al, 1997).
Angina pectoris
Swiss medical doctors stated in their study higher chances of the appearance of symptoms of Prinzmetal’s angina during early morning hours. These researchers directly concluded, in their abstract (click the link below) that overbreathing could cause vasoconstriction of coronary arteries (Jacob et al, 1994).
Stroke
 Even healthy people have heavier breathing and lowered oxygenation of the brain during early morning hours, as Australian scientists from Latrobe University in Melbourne revealed. After testing health subjects, these scientists concluded that changes in CO2 (carbon dioxide) may be a contributing factor that explains the high incidence of cases of acute episodes and stroke in the morning (Cummings et al, 2007).
Even healthy people have heavier breathing and lowered oxygenation of the brain during early morning hours, as Australian scientists from Latrobe University in Melbourne revealed. After testing health subjects, these scientists concluded that changes in CO2 (carbon dioxide) may be a contributing factor that explains the high incidence of cases of acute episodes and stroke in the morning (Cummings et al, 2007).
These effects will cause symptoms of morning sickness fatigue or morning headache fatigue with possible adrenal fatigue and high morning cortisol.
Cerebral ischemia and stroke
It is not a surprise then that British researchers from the National Heart and Lung Institute (Imperial College, London) also noted an increased risk of cerebral ischemia and stroke in the morning possibly related to changes in CO2 reactivity, used as a provocation test (Meadows et al, 2005).
Similarly, Californian neurologists noticed this reduced morning response to hypercapnia in patients with stroke. These scientists also observed the increased risk of exacerbations due to stroke during the morning hours (Ameriso et al, 1994).
Diabetes mellitus

Patients with diabetes also suffer from lower oxygenation in tissues during nights. In one study, they tested 40 patients with insulin-dependent type 2 diabetes. The measurements of tissue oxygen levels and blood rheological properties were investigated during different parts of the day. The study found reduced tissue oxygenation at night and disturbance of hemorheological blood properties when a person with diabetes as sleeping (Galenok et al, 1988)
Seizures
 Japanese doctors from the Department of Pathology for the Handicapped in Ehime University warn that those who care about people with epilepsy should know about higher chances of seizures during nights. They stated that s-w paroxysms (or seizures) combined with symptoms and lasting for over four seconds were less common during the afternoon rather than the morning hours. But even higher chances of seizures were observed during sleep (Nagao et al, 1990). Since heavy breathing reduces blood supply and oxygenation of the brain, while also making nerve cells over-excited (due to a lack of CO2 that has calmative or tranquilizing nerve cell effects), it is sensible that epileptics are most likely to experience seizures during sleep (early morning hours).
Japanese doctors from the Department of Pathology for the Handicapped in Ehime University warn that those who care about people with epilepsy should know about higher chances of seizures during nights. They stated that s-w paroxysms (or seizures) combined with symptoms and lasting for over four seconds were less common during the afternoon rather than the morning hours. But even higher chances of seizures were observed during sleep (Nagao et al, 1990). Since heavy breathing reduces blood supply and oxygenation of the brain, while also making nerve cells over-excited (due to a lack of CO2 that has calmative or tranquilizing nerve cell effects), it is sensible that epileptics are most likely to experience seizures during sleep (early morning hours).
Inflammatory conditions
A marker of inflammation, C-reactive protein, was measured during different parts of the day in obese patients (Punjabi & Beamer, 2007). The conclusion of these medical scientists from the Johns Hopkins University in Baltimore was in the title of their study: C-rеactivе prCеtеin is assCеciatеd with slееp disCеrdеrеd brеathing indеpеndеnt Cеf adipCеsity. Hence, it is not just obesity, but disordered breathing at night that can lead to inflammation due to SDB (sleep-disordered breathing).
Inflammation in amnesic patients
Since inflammation can get worse during nights in many patients, is it possible that cortisol production (cortisol is one of the key hormones to fight inflammation) also decreases at night? In this study, a group of German researchers suggested that the expected (or normal) morning cortisol increase, due to circadian changes, is not present in the amnesic patients. These patients with severe global amnesia were lacking a normal cortisol rise that takes place during early morning hours (Wolf et al, 2005).
Heavy Breathing at Night: Highest Mortality Rates
 During the first trimester of pregnancy, it is common, for up to 65 percent of females to experience vomiting and/or nausea. These symptoms are described as “morning sickness” (Flaxman & Sherman, 2000). It is known that pregnancy of modern women means chronic hyperventilation. Many of these women have even heavier breathing during sleep in comparison with their usual daily chronic hyperventilation. Hence, they often experience adrenal fatigue and high morning cortisol and morning headache fatigue.
During the first trimester of pregnancy, it is common, for up to 65 percent of females to experience vomiting and/or nausea. These symptoms are described as “morning sickness” (Flaxman & Sherman, 2000). It is known that pregnancy of modern women means chronic hyperventilation. Many of these women have even heavier breathing during sleep in comparison with their usual daily chronic hyperventilation. Hence, they often experience adrenal fatigue and high morning cortisol and morning headache fatigue.
Conclusions. Most diseases appear and progress due to heavy breathing during the early morning hours. Severely sick people are most likely to die during the same time of the day (about 4-7 am). The real health of the person can be only as good, as their morning CP measured immediately after waking up. All previous tables and graphs do not reflect the full story about the healthy state of the sick people since all those measurements (minute ventilation, CP, etc.) were done during the daytime.
Causes of Heavy Breathing at Night– Mouth breathing during sleep |
Resources* Sleep positions research |
To solve the problem with morning hyperventilation (Heavy Breathing) is one of the main goals of the Buteyko breathing method.
Note. These results (about heavy breathing and critically low body oxygenation in the sick) also suggest that all our previous considerations (Graphs and Tables about the prevalence of hyperventilation in the sick, their oxygenation, etc.) underestimate the real picture. The real respiratory parameters in sick patients are worse than those that have been measured by doctors, scientists, and researchers during daytime studies and investigations.
Two main causes of heavy breathing at night and millions of deaths during sleep worldwide every year are 1) sleeping on one’s back and 2) mouth breathing at night. There are simple and specific methods or techniques to address these and other problems. The links to these methods (how-to instructions) are provided right below here as your bonus content.
* How to prevent sleeping on the back
* How to maintain a nasal breathing 24/7
[/sociallocker]
– Some other quoted medical references
Additional resources:
– Internet Deception About Ideal Sleep Positions
– Good Sleep Hygiene provides a detailed analysis of lifestyle risk factors and practical actions to prevent Sleep Heavy Breathing Effect
Mouth-Breathing Treatment – Methods and techniques to help mouth breathers.

