- Updated on November 1, 2020
![]() By Dr. Artour Rakhimov, Alternative Health Educator and Author
By Dr. Artour Rakhimov, Alternative Health Educator and Author
Cells Oxygen Level and Brain Oxygenation Depend on Breathing
 How can we increase cell oxygenation or cell oxygen levels? What is the ideal breathing pattern that provides vital organs (the brain, heart, kidneys, liver, and so on) with maximum oxygen levels? How should we breathe day and night for higher brain oxygenation?
How can we increase cell oxygenation or cell oxygen levels? What is the ideal breathing pattern that provides vital organs (the brain, heart, kidneys, liver, and so on) with maximum oxygen levels? How should we breathe day and night for higher brain oxygenation?
When we breathe more than the norm (and this is a case for over 90% of modern people – see the Homepage for the graph with 24 medical studies), the cell oxygen level is reduced and we suffer from cell hypoxia.
Indeed, during normal breathing, our arterial blood has nearly maximum oxygen saturation. Therefore, the prime effect of overbreathing is reduced CO2 content in the lungs, blood, and other body cells and tissues. Medical studies have found that hyperventilation reduces the cell oxygen level in the following vital organs:

– brain (Brown, 1953; Kennealy et al., 1980; Liem et al., 1995; Lum, 1975; Lum, 1982; Macey et al., 2007; Litchfield, 2003; Santiago & Edelman, 1986; Skippen et al., 1997; Starling & Evans, 1968; Tsuda et al., 1987)
– heart (Foex et al., 1979; Karlsson et al., 1994; Okazaki et al., 1991; Okazaki et al., 1992; Wexels et al., 1985)
– liver (Fujita et al., 1989; Hughes et al., 1979; Okazaki, 1989)
– kidneys (Karlsson et al., 1994; Okazaki, 1989)
– spleen (Karlsson et al., 1994)
– colon (Guzman et al., 1999)
– systemic or body tissues in general (Laffey & Kavanagh, 2002; Nunn, 1987).
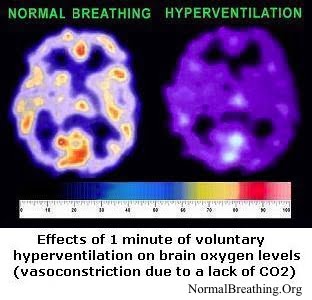
For most people, low cell oxygen levels are produced due to 2 effects that we considered before: constriction of arteries and arterioles (since CO2 is a most potent vasodilator) and the suppressed Bohr effect (less oxygen is released in tissues due to increased affinity of oxygen to red blood cells caused by hypocapnia).
These are the main effects leading to reduced cell oxygen content mentioned by many physiologists and doctors (see the quotes and references below).In particular, hyperventilation reduces brain oxygenation.
Effects of coastal breathing on cell oxygen levels
There is one additional effect that is common in modern people leading to cell hypoxia. Modern people are chest breathers (you can easily notice this). Costal breathing (or upper chest breathing) reduces arterial blood oxygen content and contributes to lowered brain and cell oxygen levels. For more information and solutions (how to develop diaphragmatic breathing 24/7), visit Effects of Chest Breathing.
Can Low Cell Oxygen Levels Appear During Hypercapnia (Abnormally High CO2)
Those people who have lung pathologies develop a more severe ventilation-perfusion mismatch that leads to critically low arterial blood oxygen levels. This effect takes place due to the ability of CO2 to dilate airways (bronchi and bronchioles). Significantly reduced blood oxygenation makes cell oxygen level low as well. Hence, these people also develop problems with tissue and brain oxygenation.
Conclusion. Whatever the level of carbon dioxide in the arterial blood, hyperventilation leads to reduced cell oxygen levels and low brain oxygenation.
In this video, Dr. Artour Rakhimov explains why measurements and calculations of the oxygen content in the whole body and brain are not easy even with most sophisticated devices.
References and quotes (Cell Oxygen and Hyperventilation/Hypocapnia)
Section “Physiologic and Biochemical Consequences”
“There is a decrease in cerebral oxygen tension based on both the Bohr effect and the decreased cerebral blood flow.”
Brashear RE, Hyperventilation Syndrome, Lung, 1983, 161: p. 257-273.
Division of Pulmonary Medicine, Indiana University School of Medicine, University Hospital, Indianapolis, Indiana 46223, USA
Section “Neurologic Effects of Hypocapnia”
“Systemic hypocapnia results in cerebrospinal fluid alkalosis, which decreases cerebral blood flow, cerebral oxygen delivery, and to a lesser extent, cerebral blood volume.”
Laffey JG & Kavanagh BP, Hypocapnia, New England Journal of Medicine 2002, 347(1) 43-53.
“Because both hypocapnia and alkalosis cause a leftward shift of the oxyhemoglobin dissociation curve, off-loading of oxygen at the tissue level is restricted. In addition, hypocapnia causes systemic arterial vasoconstriction, decreasing the global and regional oxygen supply, and compounding the reduction in the delivery of oxygen to tissue.”
Laffey JG & Kavanagh BP, Hypocapnia, New England Journal of Medicine 2002, 347(1) 43-53.
“First consider the immediate effects of hypocapnia. The most striking direct effect is on the cerebral circulation. Carbon dioxide is the most important regulator of cerebral vascular tone. Hypocapnia causes immediate vasoconstriction leading to cerebral hypoxia.”
Lum LC, Hyperventilation: The Tip and the Iceberg, Journal of Psychosomatic Research, 1975, Vol. 19, pp. 375-383.
“Furthermore, carbon dioxide controls the caliber of cerebral arteries. Hypocarbia causes vasoconstriction, and hence cerebral hypoxia. This hypoxia is augmented by a shift to the left of the hemoglobin dissociation curve for oxygen (Bohr effect), which diminishes both the amount and the rate of transfer of oxygen to tissues.”
Lum LC, Hyperventilation and Anxiety State, Journal of the Royal Society of Medicine, 1981 (74) 1-4.
Related pages:
– How to measure and increase whole body and brain oxygen with DIY tests and breathing retraining
– Oxygen extraction in lungs is connected with breathing patterns
– Breathing pattern for maximum brain oxygen levels
– Oxygen and CO2 transport
– Cerebral hypoxia is often caused by hyperventilation
– Oxygen bars and toxicity of pure oxygen.
Medical references
Brown EB, Physiological effects of hyperventilation 1953, Physiol Rev 33:445-471.
Foex P, Ryder WA, Effect of CO2 on the systemic and coronary circulations and on coronary sinus blood gas tensions, Bulletin of European Physiopathology and Respirology, 1979 Jul-Aug; 15(4): p.625-638.
Fujita Y, Sakai T, Ohsumi A, Takaori M, Effects of hypocapnia and hypercapnia on splanchnic circulation and hepatic function in the beagle, Anesthesia and Analgesia, 1989 Aug; 69(2): p. 152-157.
Guzman JA, Kruse JA., Gut mucosal-arterial PCO2 gradient as an indicator of splanchnic perfusion during systemic hypo- and hypercapnia, Crit Care Med 1999; 27: p. 2760-2765.
Hashimoto K, Okazaki K, Okutsu Y., The effects of hypocapnia and hypercapnia on tissue surface PO2 in hemorrhaged dogs, [Article in Japanese], Masui, 1989 Oct; 38(10): p. 1271-1274.
Hughes RL, Mathie RT, Fitch W, Campbell D., Liver blood flow and oxygen consumption during hypocapnia and IPPV in the greyhound, Journal of Applied Physiology, 1979 Aug; 47(2): p. 290-295.
Kennealy JA, McLennan JE, Loudon RG, McLaurin RL., Hyperventilation-induced cerebral hypoxia, Am Rev Respir Dis 1980, 122: p. 407-412.
Laffey JG, Kavanagh BP., Hypocapnia, N Engl J Med. 2002 Jul 4;347(1):43-53.
Liem KD, Kollee LA, Hopman JC, De Haan AF, Oeseburg B., The influence of arterial carbon dioxide on cerebral oxygenation and hemodynamics during ECMO in normoxaemic and hypoxaemic piglets, Acta Anaesthesiolica Scandanavica Supplement, 1995; 107: p.157-164.
Litchfield PM., A brief overview of the chemistry of respiration and the breathing heart wave, California Biofeedback, 2003 Spring, 19(1).
Lum LC., Hyperventilation: The tip and the iceberg, Journal of Psychosomatic Research, 1975, Vol. 19, pp. 375-383.
Lum LC., Hyperventilation and Anxiety State, Journal of the Royal Society of Medicine 1981 (74) 1-4.
Macey PM, Woo MA, Harper RM, Hyperoxic brain effects are normalized by addition of CO2, PLoS Medicine, 2007 May; 4(5): p. e173.
Nunn JF., Applied respiratory physiology, 1987, 3rd ed. London: Butterworths.
Okazaki K, Okutsu Y, Fukunaga A, Effect of carbon dioxide (hypocapnia and hypercapnia) on tissue blood flow and oxygenation of liver, kidneys and skeletal muscle in the dog, Masui, 1989 Apr, 38 (4): p. 457-464.
Okazaki K, Hashimoto K, Okutsu Y, Okumura F, Effect of arterial carbon dioxide tension on regional myocardial tissue oxygen tension in the dog, [Article in Japanese], Masui, 1991 Nov; 40(11): p. 1620-1624.
Okazaki K, Hashimoto K, Okutsu Y, Okumura F, Effect of carbon dioxide (hypocapnia and hypercapnia) on regional myocardial tissue oxygen tension in dogs with coronary stenosis, [Article in Japanese], Masui, 1992 Feb; 41(2): p. 221-224.
Skippen P, Seear M, Poskitt K, et al., Effect of hyperventilation on regional cerebral blood flow in head-injured children, Crit Care Med 1997, 25: p. 1402-1409.
Tsuda Y, Kimura K, Yoneda S, Hartmann A, Etani H, Hashikawa K, Kamada T, Effect of hypocapnia on cerebral oxygen metabolism and blood flow in ischemic cerebrovascular disorders, Eur Neurol. 1987; 27(3): p.155-163.
Wexels JC, Myhre ES, Mjos OD, Effects of carbon dioxide and pH on myocardial blood flow and metabolism in the dog, Clin Physiol. 1985 Dec; 5(6): p.575-588.

