- Updated on September 13, 2020
![]() By Dr. Artour Rakhimov, Alternative Health Educator and Author
By Dr. Artour Rakhimov, Alternative Health Educator and Author
- Medically Reviewed by Naziliya Rakhimova, MD
What Cramps Causes in Leg and Other Muscle Spasms?
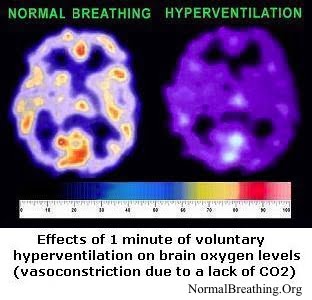 Clinical experience of Russian medical doctors suggests that people with normal body-oxygen levels do not experience any types of cramps and spasms, including foot cramps, leg muscle cramps, stomach spasm and so forth. During hyperventilation, less O2 and CO2 is available to body cells (Brown et al, 1953). An additional cause of muscle spasms is an electrical charge of the human body.
Clinical experience of Russian medical doctors suggests that people with normal body-oxygen levels do not experience any types of cramps and spasms, including foot cramps, leg muscle cramps, stomach spasm and so forth. During hyperventilation, less O2 and CO2 is available to body cells (Brown et al, 1953). An additional cause of muscle spasms is an electrical charge of the human body.
Low levels of CO2 and O2 cause overexcitement of nerve cells and involuntary contraction of muscle fibers (Brown et al, 1953; Macefield et al, 1991; Schwartz et al, 1993; Seyal et al, 1998, Sparing et al, 2007.
Therefore, overbreathing causes those effects in muscle and nerve cells that are directly responsible for cramping. You can use a simple breathing exercise that eliminates spasms in legs and other muscles in about 1-2 minute (see the link below).
Why are cramps so common in modern people and were very rare some 60-90 years ago? This graph explains the major reason behind cramps in the contemporary population.
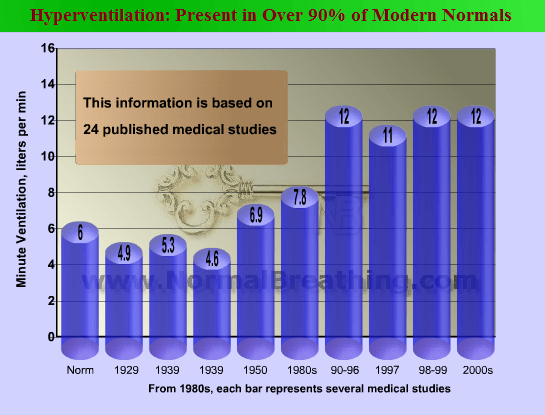
We can see that modern people are hyperventilators or they have fast and deep breathing. The situation in people with diseases even worse (see links below). Breathing more than the medical norm reduces oxygen and carbon dioxide content in body cells. The next graph provides the exact mechanism of cramps.

What Cramps Causes in Leg and Other Muscle Spasms?
Hence, effective treatment of cramps and spasms should be based on learning such automatic breathing patterns that increase levels of CO2 and O2 in the muscles of legs, feet, and stomach. Breathing retraining involves breathing exercises (or a lot of physical exercise with nose breathing) and lifestyle changes. As we see below, with over 40 seconds for the body-oxygen test, muscle spasms are virtually impossible.
Most contemporary people carry a large (hundreds of volts) positive electrical charge (indicating electron deficiency) that interferes with work of muscles that require only some fraction of a volt. Grounding is a very effective method to normalize potential of the human body. You can learn more about this cause of cramps on pages devoted to Earthing and How to ground yourself.
Nearly all people (who have poor diet) cannot get rid of their cramps due to a lack of a certain unknown-yet chemical in vegetables. This deficiency is an additional cause of cramps. These vegetables (that contain this substance) are usually dark (i.e., green or brown), such as broccoli, lentils (green and brown lentils) and beans (but not from cans or jars).
You can try this natural home remedy and solution for spasms. Other foods, like leafy greens (spinach, green or red lettuces, and so on) can help as well. Try eating them for 1-2 days and monitor the effects.
In order to prove that abnormal breathing is the cause of spasms, one can apply a simple breathing treatment How to Get Rid of Spasms in 1-2 Minutes (easy breathing exercise).
Or you can click on the picture (on the right side) to watch the video clip “How to Get Rid of Your Cramps in 1-2 min (Easy Breathing Exercise)”.
The video provides instructions for this simple breathing cure that eliminates most cramps in about 1 minute. However, some people require additional methods described on this page.
![]() Deficiencies in minerals (calcium, magnesium, sodium, and potassium) make spasms in muscles more frequent and severe. Learn methods and ways how to check and correct these nutritional deficiencies: Major Nutrients Guide for Body Oxygenation. Lack of nutrients is an additional factor that leads to cramps.
Deficiencies in minerals (calcium, magnesium, sodium, and potassium) make spasms in muscles more frequent and severe. Learn methods and ways how to check and correct these nutritional deficiencies: Major Nutrients Guide for Body Oxygenation. Lack of nutrients is an additional factor that leads to cramps.
Right below here is a table that provides a link between breathing patterns (exact numbers) and chances of cramps. This Table is provided as your bonus content.
How automatic-breathing parameters relate to spasms and cramping
(muscle, stomach, leg cramps in bed; periods or menstrual cramps; and many other types)
| Respiratory Frequency* | Body Oxygen Test (morning result) |
Chances of cramps |
| More than 20 breaths/min | Less than 20 s | Very possible |
| 15-20 breaths/min | 20-30 s | Possible |
| 12-15 breaths/min | 30-40 s | Very rare |
| 12 or less breaths/min | > 40 s | Virtually impossible |
* You cannot measure your respiratory frequency just by counting it (more info: Breathing rates)
. [/sociallocker]
References
Brown EB Jr. Physiological effects of hyperventilation. Physiol Rev 1953, 33: 445–471.
Macefield G, Burke D. Paraesthesiae and tetany induced by voluntary hyperventilation. Increased excitability of human cutaneous and motor axons, Brain 1991, 114: 527–540.
Schwartz AR, Thut DC, Brower RG, Gauda EB, Roach D, Permutt S, Smith PL, Modulation of maximal inspiratory airflow by neuromuscular activity: effect of CO2, J Appl Physiol. 1993 Apr; 74(4): 1597-605.
Seyal M, Mull B, Gage B. Increased excitability of the human corticospinal system with hyperventilation. Electroencephalogr Clin Neurophysiol, 1998, 109: 263–267.
Sparing R, Dafotakis M, Buelte D, Meister IG, Noth J, Excitability of human motor and visual cortex before, during, and after hyperventilation, J Appl Physiol. 2007 Jan; 102(1): 406-11.
Institute of Neuroscience and Biophysics, Department of Medicine, Research Centre Juelich, Juelich, Germany.
In humans, hyperventilation (HV) has various effects on systemic physiology and, in particular, on neuronal excitability and synaptic transmission.
However, it is far from clear how the effects of HV are mediated at the cortical level. In this study we investigated the effects of HV-induced hypocapnia on primary motor (M1) and visual cortex (V1) excitability. We used 1) motor threshold (MT) and phosphene threshold (PT) and 2) stimulus-response (S-R) curves (i.e., recruitment curves) as measures of excitability. In the motor cortex, we additionally investigated 3) the intrinsic inhibitory and facilitatory neuronal circuits using a short-interval paired-pulse paradigm.
Measurements were performed before, during, and after 10 min of HV (resulting in a minimum end-tidal Pco(2) of 15 Torr). HV significantly increased motor-evoked potential (MEP) amplitudes, particularly at lower transcranial magnetic stimulation (TMS) intensities. Paired-pulse stimulation indicated that HV decreases intracortical inhibition (ICI) without changing intracortical facilitation.
The results suggest that low Pco(2) levels modulate, in particular, the intrinsic neuronal circuits of ICI, which are largely mediated by neurons containing gamma-aminobutyric acid. Modulation of MT probably resulted from alterations of Na(+) channel conductances.
A significant decrease of PT, together with higher intensity of phosphenes at low stimulus intensities, furthermore suggested that HV acts on the excitability of M1 and V1 in a comparable fashion. This finding implies that HV also affects other brain structures besides the corticospinal motor system. The further exploration of these physiological mechanisms may contribute to the understanding of the various HV-related clinical phenomenona.

