- Updated on August 1, 2019
![]() By Dr. Artour Rakhimov, Alternative Health Educator and Author
By Dr. Artour Rakhimov, Alternative Health Educator and Author
 What is the cause of cystic fibrosis (CF)? The cause of cystic fibrosis on the cellular level is tissue hypoxia or low oxygen levels in body cells. This makes complete sense since ionic pumps require oxygen, and it has been known for decades that chloride and other pumps are ineffective in conditions of tissue hypoxia even in normal people (Clerici & Matthay, 2000; Karle et al, 2004; Mairbaurl et al, 1997; Mairbaurl et al, 2002).
What is the cause of cystic fibrosis (CF)? The cause of cystic fibrosis on the cellular level is tissue hypoxia or low oxygen levels in body cells. This makes complete sense since ionic pumps require oxygen, and it has been known for decades that chloride and other pumps are ineffective in conditions of tissue hypoxia even in normal people (Clerici & Matthay, 2000; Karle et al, 2004; Mairbaurl et al, 1997; Mairbaurl et al, 2002).
However, there are even more specific findings. It was recently discovered that CFTR mutation gene (cystic fibrosis transmembrane conductance regulator) is controlled by levels of oxygen in body cells in a dose-dependent manner (Bebk et al, 2001; Guimbellot et al, 2008; Yeger et al, 2001; Zheng et al, 2009).
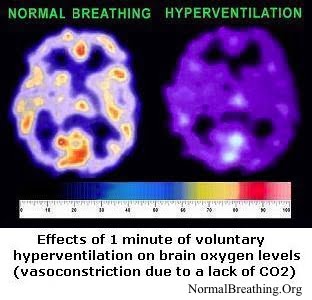 These revolutionary discoveries force us to reconsider the real causes of cystic fibrosis. It is not just a genetic disease. The advance of cystic fibrosis requires low oxygen levels. Normal oxygen levels do not allow development of the thick mucus and respiratory infections, which are the main symptoms of cystic fibrosis. What is the cause of low body oxygenation in people with cystic fibrosis?
These revolutionary discoveries force us to reconsider the real causes of cystic fibrosis. It is not just a genetic disease. The advance of cystic fibrosis requires low oxygen levels. Normal oxygen levels do not allow development of the thick mucus and respiratory infections, which are the main symptoms of cystic fibrosis. What is the cause of low body oxygenation in people with cystic fibrosis?
All available medical evidence has shown the presence of chronic hyperventilation in CF patients. Medical research has also confirmed the injurious effects of alveolar hypocapnia on lung tissue. Furthermore, medical doctors from the Department of Medicine, University of Texas Health Science Center in Houston in their publication “Importance of respiratory rate as an indicator of respiratory dysfunction in patients with cystic fibrosis” observed that “Respiratory frequency was increased in the patients with cystic fibrosis compared with a group of healthy control subjects, as was minute ventilation and mean inspiratory flow. Respiratory frequency was a sensitive predictor of respiratory dysfunction” (Browning et al, 1990).
Minute ventilation in cystic fibrosis patients at rest
| Condition | Minute ventilation |
Number of patients |
References |
| Normal breathing | 6 L/min | – | Medical textbooks |
| Healthy subjects | 6-7 L/min | >400 | Results of 14 studies |
| Cystic fibrosis | 15 L/min | 15 | Fauroux et al, 2006 |
| Cystic fibrosis* | 13 (�2) L/min | 10 | Bell et al, 1996 |
| Cystic fibrosis | 10 L/min | 11 | Browning et al, 1990 |
| Cystic fibrosis | 11-14 L/min | 6 | Tepper et al, 1983 |
| Cystic fibrosis* | 10 L/min | 10 | Ward et al, 1999 |
| CF and diabetes* | 10 L/min | 7 | Ward et al, 1999 |
| Cystic fibrosis | 16 L/min | 7 | Dodd et al, 2006 |
| Cystic fibrosis | 18 L/min | 9 | McKone et al, 2005 |
Click here for all Cystic Fibrosis References
 Development of cystic fibrosis occurs when the body oxygen level drops below 20 seconds (e.g. even if it only drops this low for some hours as during the early morning hours when the patients are at rest sleeping). See the links below for a description of the Control Pause (CP) as a means of assessing body oxygen levels.
Development of cystic fibrosis occurs when the body oxygen level drops below 20 seconds (e.g. even if it only drops this low for some hours as during the early morning hours when the patients are at rest sleeping). See the links below for a description of the Control Pause (CP) as a means of assessing body oxygen levels.
Note that most modern people have less than 20 s in the morning and, hence, having a genetic predisposition to cystic fibrosis means the gradual development of this fatal health condition for modern man. Poor results for the body-oxygen test (less than 20 s) cause the abnormality related to regulation of the chloride transport across epithelial cells on mucosal surfaces and this causes decreased secretion of chloride ions and increased reabsorption of sodium ions and water molecules across epithelial cells. This leads to the reduced thickness of epithelial lining fluid and lowered hydration of mucus. Hence, mucus becomes more viscous.
 In addition, as for people with bronchitis and sinusitis, less than 20 s CP means the suppressed immune system. That causes frequent infections in sinuses and lungs and chronic inflammation. As a result, during physical exercise people with cystic fibrosis often develop coughing, wheezing, chest tightness and/or breathlessness. Such clinical picture is typical for other chronic disorders (asthma, bronchitis, etc.) in conditions of cell hypoxia and elevated lactic acid on blood. Anaerobic energy production mechanism in cells is also caused by less than 20 s CP. This is the key factor that triggers the expression of the CFTR (cystic fibrosis transmembrane conductance regulator) gene. Thus, while a genetic mutation determines susceptibility to cystic fibrosis, chronic hyperventilation initiates expression of and exacerbates the disease.
In addition, as for people with bronchitis and sinusitis, less than 20 s CP means the suppressed immune system. That causes frequent infections in sinuses and lungs and chronic inflammation. As a result, during physical exercise people with cystic fibrosis often develop coughing, wheezing, chest tightness and/or breathlessness. Such clinical picture is typical for other chronic disorders (asthma, bronchitis, etc.) in conditions of cell hypoxia and elevated lactic acid on blood. Anaerobic energy production mechanism in cells is also caused by less than 20 s CP. This is the key factor that triggers the expression of the CFTR (cystic fibrosis transmembrane conductance regulator) gene. Thus, while a genetic mutation determines susceptibility to cystic fibrosis, chronic hyperventilation initiates expression of and exacerbates the disease.
 Similar pathological processes with mucosal abnormalities, due to pathological changes in CFTR, take place in the pancreas, sweat glands, GI tract, and other exocrine tissues. Instead of helping the immune system to fight pathogens, the increased viscosity of mucosal secretions slows down immune responses and promotes infections causing more severe symptoms of CF.
Similar pathological processes with mucosal abnormalities, due to pathological changes in CFTR, take place in the pancreas, sweat glands, GI tract, and other exocrine tissues. Instead of helping the immune system to fight pathogens, the increased viscosity of mucosal secretions slows down immune responses and promotes infections causing more severe symptoms of CF.
Too viscous mucus can also block small tubes that transport digestive enzymes from the pancreas to the small intestine. Enzyme deficiency causes inability to digest foods and development of pathological bacterial flora in the gut causing foul-smelling, greasy stools; constipation and distended abdomen; reduced weight and poor growth in children; and even blockage in the intestines, especially in the newborn. Digestive complications include pancreatic insufficiency, meconium ileus, peptic ulcer, rectal prolapse, and gastroesophageal reflux. Among typical hepatic involvements are fatty liver and liver cirrhosis.
Cystic fibrosis is reversible
Russian medical doctors have found that symptoms of cystic fibrosis are reversible if the person slows down his or her breathing pattern back to the medical norm and achieves more than 40 s for the body-oxygen test. So far, hundreds of Russians with cystic fibrosis reversed their health problems and achieved normal health. For more information about health zones related to the body oxygen level and typical symptoms in each zone, visit cystic fibrosis links below.
YouTube video: Trailer of the Amazon Kindle Book “Cystic Fibrosis: Defeated with Higher Body Oxygenation”
Clinical References: What Causes Cystic Fibrosis?.
Bebk Z, Tousson A, Schwiebert LM, Venglarik CJ, Improved oxygenation promotes CFTR maturation and trafficking in MDCK monolayers, Am J Physiol Cell Physiol. 2001 Jan; 280(1): C135-45.
Browning IB, D’Alonzo GE, Tobin MJ, Importance of respiratory rate as an indicator of respiratory dysfunction in patients with cystic fibrosis, Chest. 1990 Jun;97(6):1317-21
Clerici C, Matthay MA, Hypoxia regulates gene expression of alveolar epithelial transport proteins,J Appl Physiol. 2000 May;88(5):1890-6
Guimbellot JS, Fortenberry JA, Siegal GP, Moore B, Wen H, Venglarik C, Chen YF, Oparil S, Sorscher EJ, Hong JS, Role of oxygen availability in CFTR expression and function, Am J Respir Cell Mol Biol. 2008 Nov; 39(5): 514-21.
Karle C, Gehrig T, Wodopia R, Haschele S, Kreye VA, Katus HA, Bartsch P, Mairbaurl H, Hypoxia-induced inhibition of whole cell membrane currents and ion transport of A549 cells, Am J Physiol Lung Cell Mol Physiol. 2004 Jun; 286(6): L1154-60
Mairbaurl H, Wodopia R, Eckes S, Schulz S, and Bartsch P, Impairment of cation transport in A549 cells and rat alveolar epithelial cells by hypoxia, Am J Physiol Lung Cell Mol Physiol 273, 1997: L797–L806,
Mairbaurl H, Mayer K, Kim KJ, Borok Z, Bartsch P, and Crandall ED, Hypoxia decreases active Na transport across primary rat alveolar epithelial cell monolayers, Am J Physiol Lung Cell Mol Physiol 282: 2002, L659–L665,
Yeger H, Pan J, Fu XW, Bear C, Cutz E, Expression of CFTR and Cl(-) conductances in cells of pulmonary neuroepithelial bodies, Am J Physiol Lung Cell Mol Physiol. 2001 Sep;281(3):L713-21.
Zheng W, Kuhlicke J, Jackel K, Eltzschig HK, Singh A, Sjablom M, Riederer B, Weinhold C, Seidler U, Colgan SP, Karhausen J, Hypoxia inducible factor-1 (HIF-1)-mediated repression of cystic fibrosis transmembrane conductance regulator (CFTR) in the intestinal epithelium, FASEB J. 2009 Jan; 23(1): 204-13.

